Epilepsy in Kenya
It is estimated that in Kenya 2% of the population (over 1,000,000 people) have epilepsy. The chance of getting epilepsy is three times higher in Kenya than in developed countries
Many Kenyans confuse epilepsy with witchcraft, demon possession, a worm in the brain and they often think it is contagious and God’s punishment. In stead of going for reliable medical treatment, 80% of Kenyans makes use of the herbalist (Daily Nation, April 2009). Only 20% of Kenyans with epilepsy take reliable Anti-Epileptic Drugs (research KEMRI, 2008). This hinders them to equally participate in society. They are often excluded from school, work, church and other social activities. A major challenge of youth with epilepsy is to stand up for themselves and to avoid violence, unsafe sex and unplanned pregnancy. In Zambia 37% of people with epilepsy reported physical abuse from members of their household. This same research revealed that 20% of women with epilepsy have once experienced rape, against 3% of women without epilepsy. In the US, 30% of women with epilepsy got unplanned pregnancy before the age of 24 years, a higher rate than in the general population. These findings make it clear to us that the social empowerment of persons with epilepsy is a necessity rather than an addition to the medical care.
- Very interesting in meeting other people, especially youth
- Wanting to improve their welfare
- Wanting to reactivate their social lives
- One of the youth said: ‘it will help me and others to grow healthy and accept ourselves for having epilepsy’.
- Youth on the Move involves the media throughout the year to get epilepsy positively out of the shadows. Their message to the society is:Epilepsy can happen to anyone, you don’t choose to have it Also in epilepsy you can make it
- Epilepsy is not contagious, not witchcraft, not demon possession and not God’s punishment
- We need to be treated equally, epilepsy is not a reason to exclude us
Worldwide an estimation of 65 million persons is faced with the condition epilepsy (KEMRI Kilifi, 2010). The chance of getting epilepsy is almost three times higher in developing countries compared to developed countries. In Kenya, an estimated 800,000 Kenyans live with the condition and a majority of them experiences challenges to live beyond their epilepsy due to the stigmatization and lack of accessible, affordable and reliable health care provision.
Changing the top-down approach to the bottom up approach
To improve the well being of persons with epilepsy, a great number of institutions at national and international levels do research, develop policies and offer health care services with the aim to reduce the burden of epilepsy. WHO states that health systems have the duty to respond to people’s needs and expectations.Despite this responsibility of health service providers, we receive complaints from people with epilepsy at the grassroots level that their ideas are not implemented. Despite this responsibility of health service providers, we receive complaints from people with epilepsy at the grassroots level that their ideas are not implemented in the service provision. On top of that, there would be misunderstanding between the service providers and persons with epilepsy. The Kenyan ministry of Health states that “service providers never really get to know what their clients understand. Thus they often assume that what they have said, advised or given has been accepted and will be done, only to be surprised later that no change has taken place in terms of behavior or practice and therefore health outcomes”.
The consequence is that 80% of Kenyans makes use of the herbalist (Daily Nation, April 2009) and only 20% of Kenyans with epilepsy take reliable Anti-Epileptic Drugs (research KEMRI, 2008).When you go to conferences related to epilepsy, we get to hear the knowledge, experiences and opinions of doctors, researchers and policy makers. The personal views and experiences of persons with epilepsy and their ideas how to improve their lives is paid little attention to.
Youth on the Move takes the responsibility to represent people of the grassroots level at the national and international policy development level, so that their personal experiences, perceptions and proposals to the stakeholders at local, national and international levels can be used to achieve the task of health systems: to indeed respond to people’s needs and expectations.In this document you will read how we propose to take it a step farther. You will read the steps we take from the grassroots level to the international policy development level so that persons with epilepsy become designers, providers as well as receivers of the health care provision with the aim to ensure better well being for all.
Worldwide an estimation of 65 million persons is faced with the condition epilepsy (KEMRI Kilifi, 2010). The chance of getting epilepsy is almost three times higher in developing countries compared to developed countries. In Kenya, an estimated 800,000 Kenyans live with the condition and a majority of them experiences challenges to live beyond their epilepsy due to the stigmatization and lack of accessible, affordable and reliable health care provision.Changing the top-down approach to the bottom up approach To improve the well-being of persons with epilepsy, a great number of institutions at national and international levels do research, develop policies and offer health care services with the aim to reduce the burden of epilepsy. WHO states that health systems have the duty to respond to people’s needs and expectations.Despite this responsibility of health service providers, we receive complaints from people with epilepsy at the grassroots level that their ideas are not implemented in the service provision.On top of that, there would be misunderstanding between the service providers and persons with epilepsy. The Kenyan ministry of Health states that “service providers never really get to know what their clients understand. Thus they often assume that what they have said, advised or given has been accepted and will be done, only to be surprised later that no change has taken place in terms of behavior or practice and therefore health outcomes”. The consequence is that 80% of Kenyans makes use of the herbalist (Daily Nation, April 2009) and only 20% of Kenyans with epilepsy take reliable Anti-Epileptic Drugs (research KEMRI, 2008). When you go to conferences related to epilepsy, we get to hear the knowledge, experiences and opinions of doctors, researchers and policy makers.
The personal views and experiences of persons with epilepsy and their ideas how to improve their lives is paid little attention to. Youth on the Move takes the responsibility to represent people of the grassroots level at the national and international policy development level, so that their personal experiences, perceptions and proposals to the stakeholders at local, national and international levels can be used to achieve the task of health systems: to indeed respond to people’s needs and expectations.In this document you will read how we propose to take it a step farther. You will read the steps we take from the grassroots level to the international policy development level so that persons with epilepsy become designers, providers as well as receivers of the health

Epilepsy Prevention
In developing countries the chances of getting epilepsy are higher. The latest research suggests that the chances of getting epilepsy in Kenya are three times higher than in developed countries. Fortunately there are ways we can reduce the number of people affected with epilepsy.Let’s take a look at how we can contribute to reducing the chance to get epilepsy
- Increase use of maternity care: About four out of ten women nationwide give birth in a hospital (Ministry of Planning, 2008). When women give birth outside the hospital, they often do not receive the required assistance. The advantage of hospital delivery is that health care providers can identify complications in time. Once identified they may be in a position to avoid these complications which can lead to birth traumas or injuries that may cause epilepsy.
- Prevent infectious diseases: Infectious diseases such as HIV/AIDS, cerebral malaria, meningitis and tuberculosis can cause epilepsy. Taking preventive measures for these infections greatly reduces the chances of getting epilepsy. For example, sleeping under a mosquito net will reduce your chances of getting malaria.
- Head Trauma: Brain damage is one of the causes of epilepsy, therefore anything that prevents head trauma consequently reduces chances of epilepsy. About 9 out of 10 accidents worldwide occur in developing countries. Safe driving reduces the chances of accidents and consequently reduces the risk of head trauma.
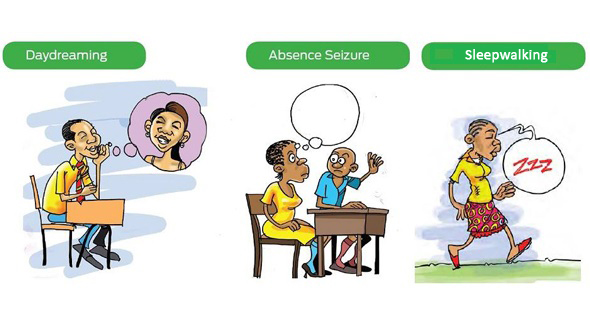
Lookalikes
- Fainting: Fainting is a temporary loss of consciousness. Unlike a seizure, the person who faints usually regains alertness soon after regaining consciousness. Fainting is caused by a temporary decrease in the brain’s blood supply. It mostly results from an abnormal reflex. The heart pumps more forcefully and the blood vessels relax, but the heart rate does not compensate fast enough to maintain the flow resulting in fainting. The main distinguishing point is that it has a short duration of loss of consciousness and that the person is not confused after the fainting.
- Psychogenic seizures: These are seizures which look like epileptic seizures, but they are caused by a psychological disturbance. One of the types of psychogenic seizures is known as hysteria. People who experience a hysteric attack often lose self-control due to an overwhelming emotion such as fear or anger. This can happen in events where crowds are excited into a state of frenzy. This may lead to mass hysteria, hyperventilating (breathing fast) and consequently the brain gets less oxygen. Once the level of oxygen goes down, people can have a seizure which looks like an epileptic seizure, when it’s really a hysteria attack.
- Breath holding spells: This could occur when a young child cries intensely, mostly after some minor upset, and holds their breath, leading to a lose in consciousness and getting limp. The attack mostly takes 30 to 60 seconds. With longer spells, the eyes might roll up; the entire body may become rigid and jerk, as the lack of oxygen to the brain actually triggers a seizure. Although the seizure looks like an epilepsy seizure, the child may not have epilepsy.
- Febrile convulsions: This is a convulsion that is caused by a rise in body temperature common among children aged 6 months to 6 years. This is not necessarily epilepsy but a temporary condition which needs to be examined by a doctor.
- Daydreaming: Daydreaming can be easily confused with an epileptic seizure; however, while lip smacking, eye blinking, or stiffening of muscle groups is common during seizures, they are not common during daydreaming. Daydreaming can be stopped by calling the person’s name,making a startling noise, touching or tickling the person. However if it is an epilepsy seizure, then the person will not respond until the seizure passes.
- Sleepwalking: During sleepwalking the person is completely unaware of what is happening, and it is understandable that people confuse it with epilepsy, as it presents like some types of seizures. It is important to know that sleepwalking can also happen to people who do not have epilepsy.
- Tics: Tics are brief, involuntary, and repetitive movements. The most common tics are eye blinks, facial grimaces, shoulder shrugs, and head movements. Although people can make the same movements during an epileptic seizure, these tics are not necessarily caused by epilepsy.
- Tourette’s syndrome: Someone with Tourette’s syndrome ha s a specific type of tic which is chronic repetitive movements and voice tics. The voice tics range from grunts and throat-clearing sounds to involuntary cursing and other embarrassing noises. These tics are also commonly confused with epilepsy.
- Diabetes: People with diabetes usually have low or high blood sugar; this can trigger a seizure which looks like an epileptic convulsive seizure. Even though the first aid they need during the convulsive seizure is the same, people with diabetes require a different medical treatment from that given to people with epilepsy.
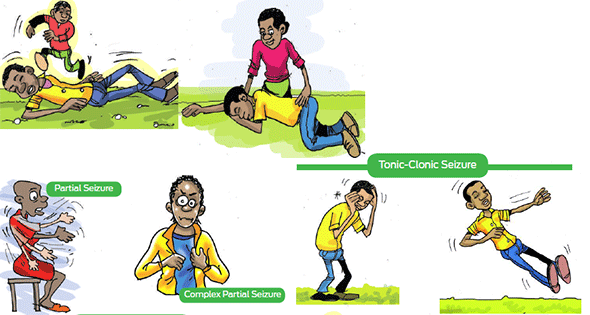
Types of Seizures
People with epilepsy have different types of seizures. One person may fall and jerk, whereas someone else may only appear absent or non-responsive for a while and stare.For some people the seizure affects only a part of the brain. This type of seizure is called a partial seizure. A generalized seizure occurs when the whole brain is affected by the seizure and one loses consciousness.Most people have only one type of seizure, but in some instances they experience several types of seizures. These include:
Partial Seizures
During a partial seizure, only a part of the brain is affected. The signs and symptoms will depend on the part of the brain where the seizure occurs and which body functions are controlled by that part of thebrain.The following seizures are partial seizures:- Simple partial seizures: In this type of seizure, the person remains conscious but experiences sensations or uncontrolled movements. The seizure can cause rhythmical twitching of one limb or a part of the limb, or unusual tastes or feelings such as pins and needles in a specific part of the body. These unusual sensations or movements are sometimes the beginning of a generalized seizure with eventual loss of consciousness;they are known as ‘warning signs’ or ‘auras’.
- Complex partial seizures: These seizures differ from simple partial seizures in that consciousness is reduced and the person will remember nothing or very little of what happened during the seizure. The seizure can begin with an odd taste in the mouth or smell like rotten eggs, a rising feeling in the stomach, or a sense of déjà vu. Then the awareness slowly reduces and the person may fiddle with clothes or objects, mumbling or wandering about in a state of general confusion. The person may respond if spoken to. The person is often tired, briefly confused after the seizure and may have a headache.
- Partial seizures secondarily generalized: These seizures start as partial seizures, then spreads to the whole brain, leading to a seizure such as the tonic-clonic seizure that involves the loss of consciousness.
Generalized Seizures
In generalized seizures, the whole of the brain is affected during the seizure and the person loses consciousness. These seizures mostly come without a warning sign (aura) and afterwards the person will not know what had happened during the seizure.
- Tonic clonic seizure: It is the most common type of seizure, also known as grand mal seizure. In the first part of the seizure, the person becomes stiff and may fall. The muscles then relax and tighten rhythmically causing the person to convulse. At the start of the seizure the person may bite their tongue or cry out. In some cases they may urinate. After the seizure they might be tired, confused, have a headache and may need some rest to recover fully.
- Absence seizure: This is common in children, also known as petit mal. The person briefly loses consciousness and doesn’t respond to anything. They appear blank and make no movements, except for maybe fluttering of the eyelids or swallowing movements. Absence seizures often last for only a few seconds and usually go unnoticed. Absence seizures are regularly confused with day dreaming. However, children who daydream tends to respond if someone pushes them or talks to them, whereas children who are experiencing an absence don’t.
- Tonic seizure: General stiffening of the muscles without rhythmical jerking is characteristic for this type of seizure. The person may fall to the ground with a consequent risk of injury, however recovery is quick.
- Atonic seizure: Also known as drop attacks, they involve a sudden loss of muscle tone, causing the person to fall. The risk of getting injured during this seizure is high, but recovery is generally quick.
- Myoclonic seizure: This involves brief and abrupt jerking of one or more limbs. This often happens within a short time of waking up. The seizures can happen on their own or with other forms of a generalized seizure

Causes
The cause of epilepsy can be defined as the initial reason for which someone has epilepsy. In many instances, the cause of the condition is a mystery. These are called idiopathic epilepsy. If the doctors have found the cause of the seizures, then we speak of symptomatic epilepsy. The following conditions can lead to epilepsy:
- Brain damage or injury: The level of brain damage or injury determines the effects on a person’s health. Sometimes the injury doesn’t bring any change in your functioning. But in some cases it can lead to physical challenges, such as epileptic seizures.
- Brain tumor:A tumor is an uncontrolled growth of a part of the body. Sometimes it’s cancerous, but sometimes it isn’t but can still cause damage by direct pressure on other tissues. Some tumors in the brain can cause epilepsy while others don’t. This means that not everyone who has a brain tumor gets epilepsy.
- Infections: Infections like cerebral malaria, meningitis, HIV/AIDS and tuberculosis can especially affect the brain and lead to epilepsy if not properly treated in time.
- Stroke: A stroke is a blood clot that blocks the vessel which carries blood from the heart to the head, or the vessel breaks open. In some cases this can lead to epilepsy.
- Birth complications: When there are complications at birth, such as prolonged labor, the baby may lack oxygen and this may lead to brain injuries. These injuries may result in epilepsy in the baby or in later life.
- Alcohol or drugs: When one takes alcohol or drugs inappropriately over a long period of time, it may harm the brain and lead to epilepsy.Inheritance: Epilepsy is generally not inherited. However, in very exceptional cases, if a high number of family members are affected with the condition then there is a risk of passing it on to their children through their genes. Whatever the cause of epilepsy, one thing is clear: nobody chooses to have epilepsy. It can happen to anyone at any age and in any community.

Triggers
These are the most common triggers. However some people have very unique triggers, like listening to a special kind of sound or eating a certain food. Exposure to triggers increases the chances of experiencing a seizure. Being well informed about these triggers can help reduce the number of seizures. For instance, if missing a meal is a prominent trigger for one person, then they understand the importance of taking meals. In time this will reduce the number of seizures.
- Lack of sleep: Getting adequate rest reduces the chances of getting seizures. This doesn’t mean staying away from activities but finding a good balance between being active in the daytime and getting adequate sleep at night to gain energy for the next day.
- Stress (anxiety and excitement): People experience negative and positive stress, both of which can provoke a seizure.
- Menstruation: There are women who have more seizures during menstruation; it is essential for them to inform their doctor about it. There are medications that can be taken during these days to reduce the number of seizures. Like other anti-epileptic drugs, they have to be prescribed by the doctor and can’t be bought over the counter. They also need to be taken every month to be effective.
- Missed meal: Missing a meal or eating later than usual can cause the body to get out of balance and could consequently trigger a seizure. It is therefore very important to eat regularly in the morning, afternoon and evening.
- Missed medication: Forgetting to take your medication or taking it a bit late can trigger a seizure. It is important to take another dose if you vomit half an hour after taking medication because the other one may not have been absorbed by the body.
- Illness: A seizure can be triggered by illnesses such as fever, fl u, malaria, and diarrhea. It is important to inform a doctor that you are being treated for epilepsy before they treat you for any other illness. This is because other drugs can affect how the anti-epileptic drugs works.
- Alcohol: When you have epilepsy, drinking alcohol may affect your body more than it does others. The alcohol usually takes effect faster and may even trigger a seizure. However, it depends on the amount you take; only a sip will not have much of an effect. It doesn’t typically provoke a seizure straight away, but about 6 to 72 hours aft er the alcohol intake. Ask yourself if the effect of the alcohol intake is worth the pleasure of drinking it.
- Illicit drugs: Cocaine, marijuana, ecstasy and others do more than only make you high for a moment. They also affect the body in the long term. For some people, taking illicit drugs leads to epilepsy. If you already have epilepsy, the illicit drugs can make your epilepsy worse as well as trigger seizures. Therefore we strongly advise you not to use illicit drugs.
- Flickering lights or patterns: Only 3% to 5% of people with epilepsy are sensitive to flickering lights or patterns. This may be when they watch television, work on the computer, or sit under a tree where the sunlight shines through the leaves as the wind rustles them.
- Overheating: Staying in the sun for long can cause a body to overheat and can lead to a seizure for people with epilepsy. This doesn’t mean that one has to stay indoors all the time to avoid the warm sunshine. When it’s very warm indoors, then catch a fresh breeze outside. If overheating is a major trigger, find ways to get fresh air. You can also consider protecting your head from the warm sun with a hat, just as walking in the shade can keep you fresh.
It’s important to understand that these triggers cannot give you epilepsy. They can only provoke a seizure if you already have epilepsy. Triggers are not the same for everyone and it can take some time to recognize them, especially if seizures are not frequent. Although trigger reduction is crucial, it is important to know that epilepsy is not caused by it. We recommend that people with epilepsy discuss the seizures with their doctor to ensure that the medical treatment offered is the right one
.
Diagnosis
Everyone who has epilepsy, or thinks that they have epilepsy, must visit a doctor for consultation. It will help the doctor if you take someone with you who was present during your seizure, as they can explain what it looked like.The doctor will ask various questions, like:
- What do the seizure look like?
- How long do the seizures take?
- How do you feel before and after the seizure?
Usually a doctor can draw a conclusion about the types of seizures you experience from the answers given. If they are still not sure, they may request medical tests such as an EEG or MRI, which give definitive information about what happens in your brain.
Electroencephalogram (EEG): An EEG is a test that records the electrical activity of the brain. Special sensors (electrodes) are attached to the head and connected by wires to a computer. The computer records the brain’s electrical activity on the screen as wavy lines. The person may be asked to hyperventilate or to look at flashing lights so as to activate brain discharges. A seizure can be seen by the changes in the normal pattern of the brain’s electrical activity. Most EEGs can be run in about an hour or less.
Magnetic Resonance Imaging (MRI): To search for the cause of your seizures, the doctor may request for an MRI scan. The MRI takes pictures of the inside of your brains with the help of a magnetic field. The images are extremely precise, and may for example show a tumor or damage in the brain which could be the cause of the seizures. It may be necessary to get an injection (contrast) before the test, to help the MRI scans reveal more. Afterwards, you will be asked to lie down on a narrow bed. They will position cushioned pads on either side of your head to keep it still. It is important that you lie as still as possible during the test so as to get clear pictures without movements. The technician will roll the bed inside a shaped tube and they will give you guidance through each step. Once in the tube, you will not feel anything except for the cushioned pads around your head, but you will hear a series of knocking sounds. The duration of the scan depends on the area in the brain which the doctor wants to examine. This could take twenty minutes or longer.

Treatment
It is important to get treatment to control the seizures. However, the majority of people with epilepsy in Kenya do not make use of it. Research done in Kilifi reveals that, 8 out of 10 people with epilepsy don’t take anti-epileptic drugs (Edwards,2 008). Some people deliberately avoid the treatment, whereas others unintentionally don’t take drugs. Let’s take a look at reasons why people could not be taking their drugs:
- Diagnosis: The person may not have gone to the doctor for a diagnosis, or may have visited a doctor but received a miss-diagnosis. As a result, a patient may be prescribed a treatment that is meant for another condition.
- Stigma: Sometimes people who have epilepsy seizures feel embarrassed about it, and even avoid visiting the doctor. Some prefer to deny the condition rather than face the doctor.
- Doctor Mistrust: Many Kenyans have little or no confidence in the local healthcare providers due to past malpractice. According to Community Strategy 2005 many doctors do not pay proper attention when diagnosing and prescribing treatment or explaining medical conditions.
- Drug Availability: Even in the cases where epilepsy is correctly diagnosed, the availability of drugs still remains a major challenge. It is therefore important to maintain an adequate stock of the drugs.
- Finances: In developing countries where a good number of the population live under a dollar a day accessing treatment is difficult for many people.
- Ignorance: In some cases the patient doesn’t know just how essential the drugs are. But sometimes they may simply forget to take the medication
- Side effects: Anti-epileptic drugs usually have extensive side effects; in an effort to alleviate these side effects some may possibly stop taking the medication all together.
- Rebellion: Young people are often resistant of authority figures, more so in their teen years. For the youth with epilepsy this rebellion can have untold consequences when it leads them to skip medication.is could take twenty minutes or longer.

Treatment
When a person gets a seizure, they can be offered support to reduce the burden of it. The type of first aid that needs to be given during seizures usually depends on the type of seizure. With convulsive seizures, the person administering the first aid needs to:
- Stay calm
- Remove any sharp or harmful objects or move the person away from danger
- Support or place something soft beneath the head
- Loosen any tight clothing at the neck
- Roll the person onto their side (recovery position) when jerking stops
- Stay with the person until fully recovered and oriented
- Seek medical help if the seizure takes longer than 5 minutes
- Know the don’ts
- Do not restrain the person when they’re jerking, it can cause bruises
- Do not put anything in the mouth, you cannot prevent the person from biting their tongue
- Do not give food or drinks before the person is fully recovered as they might choke on it
- If the person experiencing the seizure is on a wheelchair or car seat, they can remain seated if secure and safely strapped in.
- When the seizure is happening it is important to support the head. When the jerking stops and they are still unconscious, they can be removed from the seat and rolled on their side to allow excess saliva to come out.

